
![]()
The Deadly Adenovirus and Klebsiella pneumoniae
by Donna Dick
This is going to be VERY long...but if you are a breeder, you need to take time to read this article. This knowledge could very well end up saving your entire litter someday. Lord how I wish I knew then what I had to learn the hard way.
My Mastiff bitch, Baby, delivered a litter of 14 pups on July 23. All pups survived and were doing well. Within 24 hours I lost a puppy. She was perfectly healthy in every way. She had just nursed and was doing fine, but the very next minute she was dead. I was sitting "in" the whelping box feeding other pups when she died. No symptoms, she just died.
We performed a necropsy and the vet said he thought the dam had laid on her because her lungs looked bruised. I accepted this, though could not understand how it could have happened. A friend had come to help with the whelping. She and I never took our eyes off of the whelping box. But with 14 pups, ok, maybe we miss counted the pups, it could've happened. All other pups were doing great, eating normally, and thriving. The only symptoms we ever saw at all was that at times they would aspirate as they nursed, even when they nursed on the dam.
When the pups were 3 weeks of age I notice one pup just sitting up and hanging his head. He would not lie down. When I checked him he seemed ok. He nursed, just would not lie down. He appeared to have difficulty breathing when picked up. Within 4 hours he was in death gasp.
We rushed him to the vet and took x-rays. The vet said it appeared as if his lungs were crushed. The dam must have laid on him because the X-rays showed bruised and bleeding lungs. The pup was put on antibiotics and I was told to watch him.
That evening, approximately 7:00 PM, another pup came down with similar symptoms. Just sitting up and hanging his head. I knew then we were looking at something that was about to go through the whole litter unless we did something NOW! I called the vet and he started the whole litter on antibiotics.
The next morning the first pup died. The second was in serious trouble, and I had 2 more affected pups.
I took the dead puppy in for necropsy and the others in for exam. I attended the necropsy and, indeed, the pup's lungs looked bruised. Blood had infiltrated the lungs. Not pooled like pneumonia (so it could be drawn off) but it appeared as if the capillaries were bleeding. No other organs appeared affected. They were all absolutely normal and well formed. We took a culture and sent it, and all internal organs to the State Lab. The sad thing was the results of the culture would not be back for 7-10 days and from the time the pup went symptomatic within 24 hours it was dead. This left us NO time to wait to find out what we were dealing with !!!
We started the whole litter on aggressive preventative medicine. We had NO idea what to treat them "with", so we battered them with everything veterinary science had to offer. The whole litter was put on Clavamox orally, Ampicillian via injection twice/day, Cephalexin orally, Vitamin C to boost their immune system, Vitamin K via injection to control bleeding, and Dialex G to open breathing passages.
The morning of the second day I attempted to tube feed a pup because he was too weak to eat. As I placed the tube into his throat he faded. I was positive it was placed in the esophagus not the airway. All resuscitation attempts failed. This pup was put on ice and sent off to the state lab for a complete autopsy.
Neither of the 4 vets in the clinic had a clue what this was. We suspected they got some bad formula and had been poisoned. The thing was, most of the pups had the same batch of formula but not all the pups were affected. So I sent a sample of the formula off to the state Lab for testing. To date I do not have the results from those tests.
During this time my vet burned the midnight oil searching through medical journals and calling every major teaching hospital and State Lab in the USA. NO ONE had a clue what this was. I called every professional mind I could think of from a virologist to a toxicologist. Again,....NO one had a clue! The pup's symptoms simply did NOT fit into any particular category of known disease.
Symptoms were as follows:
1st - Sitting up hanging head, will not lie down.
2nd - (within 2 hours) Labored breathing
3rd - (4 hours after first symptom) death gasp requiring oxygen mask to breathe
4th - (20 - 24 hours) death
Since we had NO idea what we were dealing with I kept the affected pups away from the healthy pups. In case it was a virus, I disinfected the entire house and bleached all bedding and floors. We changed clothes before going from well pups to sick pups and my hands were so raw from washing them with antibacterial solution and alcohol that they bled.
A friend lent me an oxygen condenser and I rented oxygen tanks for the sick puppies for oxygen masks ($15 per day). My house became a hospital with IV drips and oxygen tents. Even though the affected pups were put in oxygen tents I had to watch them VERY closely because if they began gasping I had to pull them out of the tent and put an oxygen mask directly over their muzzle or they could not breathe.
Since the pups could not nurse I attempted tube feeding. But, just as the 2nd pup I lost, tube feeding was not an option because as I "began" insertion of the tube the pup would fade. So we kept the affected pups going with 50 CC's Dextrose subcutaneous injections twice per day.
My husband had to work so this left me to care for the pups on my own. I was averaging 2 hours sleep per day for two solid weeks. Some days I would go for three whole days without even sitting down because I knew if I ever sat down I'd fall asleep and my pups would die.
To lighten the mood of this story I'll tell on myself about the time I was standing up leaning on the kitchen table with my eyes glued to the oxygen tent and the next thing I knew I hit the floor. I fell asleep standing up and landed top of Baby, who was not impressed by the way. She looked at me like "Mom, are you nuts?".
The first 24 - 48 hours were critical. But here is the turning point. I was walking the floor with one of the pups holding an oxygen mask on its muzzle, (crying and praying out loud to God to save my babies), and rubbing the puppy's throat when God gave me the answer. The pup's throat was swollen. No one noticed this before because the swelling was in the esophageal region, not in the lymph nodes nor tonsils. They couldn't breathe because the breathing pathways and esophagus was swollen shut. Thus the reason tube feeding caused the puppy to fade. The tube completely closed off the airway.
It just so happened at this time my husband was at the vet picking up more antibiotics. I called the vet and told him what the good Lord had shown me. (Boy this sure made me a believer in the power of prayer!)
The vet prescribed something that you "never" give a puppy. He gave us Cortisone. The vet did not want to prescribe it, but as he said, "at this point, what choice do we have?". We were told to give one injection that day (only to the affected puppies), wait 48 hours and give a second injection "IF" they needed it, but no more.
That was the turning point. Within 24 hours of the first injection the pups would lick about a teaspoon of thin gruel from my fingers. Within 48 hours they would lick about 1/4 cup from a flat dish. Within 72 hours they ate about a half cup of gruel and nursed on the dam for 5-10 minutes. They were rapidly showing improvement.
After the first week we decided that the preventative medicine had to be working because we had no new symptomatic pups and the affected pups were showing improvement. The thing was...we had NO idea "which" medicine was working, so we had to keep them on everything.
Now, here is what you’ve been waiting for.
Ten days after the culture was sent off we received Lab results. They are as follows:
PATHOLOGY:
This is the fresh carcass of a male Mastiff puppy in good nutritional condition. The subcutaneous tissue of the ventral abdomen is very watery. The spleen is approximately 2 times normal size and very dark. The lungs fail to collapse and are mottled gray to red. The parenchyma (cells in a tissue or tissues in an organ that are concerned with function) is slightly firm and large portions sink in formalin.
Morphologic Diagnosis:
Lung - Severe locally extensive bronchopneumonia
Spleen - Splenomegaly (Definition: An enlargement of the spleen beyond its normal size.)
Diagnosis:
Canine Adenoviral pneumonia with secondary bacterial (Klebsiella) infection
Antimicrobial Susceptibility:
Organism - Klebsiella pneumonia
Amikacin: susceptible Ampicillian: resistant
Amox/Clavul: susceptible Bacitracin: resistant
Ceftiofur: susceptible Clindamycin: resistant
Cephalothin: susceptible Erythromycin: resistant
Chloramphenicol: susceptible Sulfadimethox: resistant
Enrofloxacin: susceptible Vancomycin: resistant
Gentamicin: susceptible
Kanamycin: susceptible
Neomycin: susceptible
Orbifloxacin: susceptible
Tetracycline: susceptible
Trimeth/sulfa: susceptible
The lab results diagnosed Canine Adenovirus Type 2 infection with a secondary bacterial infection of Klebsiella. Now the peculiarity of it was that none of the pups showed ANY symptoms of Adenovirus. No fever, no runny eyes or nose, no diarrhea, no vomiting. The only symptoms were those listed previously. Seven days after the onset of the puppies’ symptoms the dam came down with a slight temperature for 48 hours. No other symptoms. It is suspected she, too, was affected. But due to the fact she was an adult, and she had been put on Cephalexin following her C-section, her system had some antibodies to prevent serious illness.
I believe it is important to note that the dam had been fully vaccinated five (5) weeks before being bred. The vaccine did contain Adenovirus Type 2 and I made sure that all pups nursed from the dam prior to bottle feeding. My only guess is that either the vaccine was bad, or she did not develop the necessary antibodies from the vaccine. I have vowed to never again breed a bitch without doing titers first.
The dam had not been off premises prior to, nor following her C-section. Neither had any of our other dogs been off our premises, nor stray dogs on our property within the confines of the fenced area where the dam ventured. We took special care to change clothes and wash after returning from the vet to pick up Puppy Formula. So we do not know how the virus was introduced.
After much diligence, many tears, loss of sleep, a wonderful caring veterinarian, and pure determination; eleven (11) pups out of fourteen (14) survived. A total of seven (7) pups were affected. We lost three(3), three(3) were severely ill, and (1) just symptomatic for twenty four (24) hours. The other pups were never symptomatic. The most likely reason the other pups did not become symptomatic is because of aggressive preventative medicine.
All eleven (11) surviving pups are doing extremely well. At eight(8) weeks of age ten(10) of the pups passed their veterinary exams with flying colors. During the exam I requested Specific Gravities, and BUN on the pups whose Specific Gravities were questionable. The one puppy who had some remaining congestion also had chest X-rays. They have all been declared healthy except for one male who has some minor lung damage. At twelve weeks of age he was declared healthy and the vet said he should live a normal, healthy life.
During this ordeal, in my search for answers, I spoke with another breeder who reported she had a litter of thirteen (13) with the "very exact same symptoms"; she lost her entire litter. Neither necropsies nor cultures were performed so she never did find the cause.
I posted this article on the Mastiff Breeder list and requested it to be forwarded to other Breed lists. I have received phenomenal response from other breeders of all breeds who have lost entire litters to this horrid illness and no one knew what it was or how to treat it. Many letters of thanks have flooded into my email. One month after my ordeal my vet reported to me that a litter of Boxer pups was brought in with the exact same symptoms. Because of our recent experience, the vet knew how to treat it.
An important note: Clorox Disinfecting Spray kills 99% of most bacteria for up to 24 hours and also kills Adenovirus Type 2.
I wish to extend my eternal gratitude to a dedicated and conscience veterinarian, Dr. Steven Crews DVM, at the Reelfoot Animal Hospital. Without his dedication, diligence, and hard work I would never have saved my litter.
I apologize for this being such a long report, but I hoped to share this with you so if you ever see similar symptoms you will know what to look for and how to treat it to save your litter. Knowledge is Power !!!
Donna Dick
Mastiffs Of Grandeur
Canine Adenovirus
1
Adenovirus (ADD-no-VY-rus)2
CANINE ADENOVIRUS TYPE 2 - infections are primarily respiratory, evidenced by pneumonia, bronchitis, tonsillitis, and pharyngitis. CAV-2 has not been associated with corneal opacity ("blue eyes"), uveitis or virus localization in the kidneys, which may be characteristic of canine adenovirus type 1 (CAV-1) infections.3
Adenovirus Type 2: Canine adenovirus type 2 infection causes respiratory disease which in severe cases may include pneumonia and bronchopneumonia. It has also been demonstrated that the canine adenovirus type 2 vaccine cross protects against hepatitis (adenovirus type 1).3
Tracheobronchitis: (kennel cough) This disease can be caused by many different bacterial agents, such as, adenovirus type 2, canineadenovius type 1, canine parainfluenza, and Bordetella brochiseptica. These highly contagious, air-borne agents cause mild to severe inflammation of the trachea, bronchi and lungs.A B
4
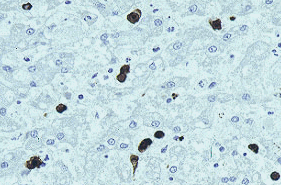
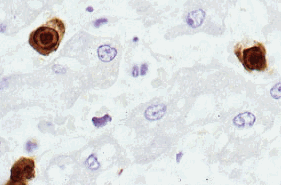
A) Liver, dog. Natural infection with canine adenovirus (infectious canine hepatitis virus). Intense, mostly nuclear, staining of sinusoidal cells and occasional hepatocytes. Immunoperoxidase-DAB for adenovirus.4
B) Staining of intranuclear inclusion bodies. Immunoperoxidase-DAB for adenovirus.5
Adenovirus-2 causes canine infectious hepatitis, which is a disease of the liver and other body organs. It is a quick killer and death may follow even two hours after the onset of symptoms.6
Respiratory infections rarely involve a single infectious organism, and there is often secondary infection with bacteria such as Staphylococci, Streptococci, Pasteurella and E.coli. Again, it is important to use a disinfectant with proven activity against the range of possible pathogens.7
Adenovirus (aka H= hepatitis): There are 2 types of adenovirus viruses. Both can cause several different types of liver disease (both acute and chronic hepatitis). Adenovirus 1 causes stillbirth in puppies. Although these viruses aren’t very common, they have potentially serious consequences and can be prevented easily through vaccination. Standard vaccines only protect against Type 2, which is more severe.8
Parainfluenza and Canine Adenovirus-2 are highly infectious diseases of the respiratory tract. They are transmitted by air, and readily cause localized infections.9
Mostly found in towns and cities, but foxes can be carriers. Young dog disease (<12 months). The virus is excreted in saliva, faeces and urine, and infection is usually by mouth. The virus is not very hardy but can survive up to 10 days in sheltered conditions. The virus incubates for 5-7 days, then some dogs recover but in others there is widespread liver damage, leading to jaundice, and fluid in the abdomen and chest (effusions). Signs are vomiting and fever with very severe abdominal pain. The cornea can be damaged leading to "Blue-eye."Treatment is fluids and supportive treatment including vitamin / amino acid supplementation (Duphalyte fluid). Vaccination is with either killed vaccines or with a live related vaccine Canine AdenoVirus 2, hence some vaccines contain "H" and some "A2" as their hepatitis protection.
REFERENCES:
1- http://www.petnet.com/pfido/disease.asp
2- http://www.dresslersdog.com/store/diseases.html
3- http://www.spiritone.com/~visions/info.html
4- http://www.cvm.missouri.edu/vmdl/ramos/IHC/IHC_tests_available/Adenovirus/body_adenovirus.html
5- http://www.luckyones.com/luckyones/luckdogvet.htm
6- http://www.antecint.co.uk/main/vet3.htm
7- http://www.brebt.com/nls/nl1200/nl1200.html
8- http://dogsindia.com/infectious_diseases.htm
9- http://www.avonvets.co.uk/2ndyr_hands/Canine_inf_dis.html
1
KLEBSIELLA: ONE POTENTIALLY NASTY BACTERIAAs you may know, we all have millions of bacteria in our gastrointestinal tracts, primarily in the colon (or "large" bowel). These bacteria are important for normal bowel health and function. Klebsiella is the genus name for one of these bacteria. When Klebsiella bacteria get outside of the gut, however, serious infection can occur.
As a general rule, Klebsiella infections tend to occur in people with a weakened immune system. Many of these infections are obtained when a person is in the hospital for some other reason. The most common infection caused by Klebsiella bacteria outside the hospital is pneumonia.
Klebsiella pneumonia tends to affect people with underlying diseases, such as alcoholism, diabetes and chronic lung disease. Classically, Klebsiella pneumonia causes a severe, rapid-onset illness that often causes areas of destruction in the lung.
Infected persons generally get high fever, chills, flu-like symptoms and a cough productive of a lot of mucous. The mucous (or sputum) that is coughed up is often thick and blood tinged and has been referred to as "currant jelly" sputum due to its appearance.
Mortality in Klebsiella pneumonia is fairly high due to the underlying disease that tends to be present in affected persons. While normal pneumonia frequently resolves without complication, Klebsiella pneumonia more frequently causes lung destruction and pockets of pus in the lung (known as abscesses).
There may also be pus surrounding the lung (known as empyema), which can be very irritating to the delicate lung tissue and can cause scar tissue to form. At times, surgery may be needed to "rescue" a lung that is trapped in irregular pockets of pus and scar tissue.
Klebsiella can also cause less serious respiratory infections, such as bronchitis, which is usually a hospital-acquired infection. Other common hospital-acquired infections caused by Klebsiella are urinary tract infections, surgical wound infections and infection of the blood (known as bacteremia). All of these infections can progress to shock and death if not treated early in an aggressive fashion.
Many hospital-acquired infections occur because of the invasive treatments that are often needed in hospitalized patients. For example, intravenous catheters used for fluid administration, catheters placed in the bladder for urine drainage and breathing tubes for people on a breathing machine can all increase the susceptibility to infection.
While these devices may be needed in certain patients, they allow bacteria to bypass the natural barriers to infection and get into a person's body. The result may be an infection if the person's immune system cannot fight the bacteria. Unfortunately, the people who need invasive treatments often have weakened immune systems because of their underlying disease.
Klebsiella bacteria are generally resistant to many antibiotics, such as penicillin. Often, two or more powerful antibiotics are used to help eliminate a Klebsiella infection. Usually, a culture of the suspected infection site is required before a doctor can know that Klebsiella is the cause of the infection.
This may involve getting sputum samples (patients are asked to cough up phlegm into a jar), blood samples (using a needle to draw blood from a vein), urine samples or a swab (with a q-tip) of a surgical wound.
Once the samples are obtained, they are taken to a laboratory and put in a special substance which allows bacteria to grow (this is known as "culturing" the bacteria). If bacteria begin to grow, the lab can determine which type of bacteria it is.
If the bacteria are Klebsiella, the lab will need to run special tests to determine which antibiotics are best to treat the infection (this is known as sensitivity testing). This is important because different Klebsiella bacteria are resistant to different antibiotics, so what works for one Klebsiella infection may not work for another.
These culture and sensitivity tests may take two to three days to complete. A doctor may not wait for the test results to start antibiotics. Often, a powerful antibiotic or two is started right away once infection is suspected. The antibiotic can be switched a few days later if the results of the culture and sensitivity tests suggest a more appropriate drug to treat the infection.
Klebsiella bacteria are a part of normal life and live inside almost all of us. Although it is something we generally don't like to think about, we need Klebsiella in our colon to keep us healthy. Unfortunately, once Klebsiella escapes the gut, it can be one nasty bacteria.
2
Klebsiella pneumoniaeKlebsiella pneumoniae cell showing numerous fimbriae(or pili; type 1). They are seen only with the electron microscope and confer adhesive properties enabling the bacteria to adhere to epithelial and red blood cells, or other solid substrates. Scale bar in µm. Negative staining with uranyl acetate. (Unpublished micrograph).
REFERENCES:
1
-http://www.personalmd.com/news/klebsiella_102299.shtml2- http://www.bacteriamuseum.org/species/Kpneumoniae.shtml
![]()
![]()
Crestwood
Mastiffs — Gold
Coast Mastiffs — DeVine
Farms — Monarch
Mastiffs
![]()
Last updated May 02, 2002